Opioid Dependence Treatment (ODT) Resources

Background
Substance Use Disorder (SUD), specifically in relation to opioids, is the term used to describe persistent opioid use, despite serious harms and negative consequences. This term may also be used more broadly for other substances, including alcohol and tobacco.1
The harms associated with opioid SUD impact the individual but may also extend to the wider community. These may include:
- Loss of life through opioid overdose.
- Medical impacts, including transmission of blood borne viruses (e.g. hepatitis C, hepatitis B and HIV).
- Mental health issues, such as depression.
- Social issues, such as impacts on relationships, employment, education, housing, parenting, finances, and crime.
- Financial costs related to health, social services, and the judicial system.2
Dependence refers to the gradual physiological adaptations to the ongoing use of an opioid, which includes tolerance and the presence of withdrawal symptoms when the opioid is ceased. This may occur with prescribed opioids, as well as non-prescribed opioids used for non-therapeutic purposes.
The term “dependence” can be confusing in the context of substance use disorders. A person who is being treated by a physician with opioids (for instance in chronic pain), may develop a dependence to opioids (characterised by tolerance, dose escalation, and withdrawal symptoms) without an associated substance use disorder (characterised by continued use despite harm, seeking behaviours, and supplementation with non-prescribed opioids).
For the purposes of Opioid Dependence Treatment (ODT), a person would be referred for treatment if they have developed a substance use disorder to opioids from any source, or a dependence to opioids obtained from non-prescribed sources used in a non-therapeutic manner.
Role of Community Pharmacy
ODT aims to reduce the harms related to opioid use in the community, including the social, economic and health impacts. Community pharmacy plays a critical role in ODT, providing 85% of dosing sites nationally for people seeking treatment for opioid dependence2. Pharmacists provide treatment for methadone, sublingual buprenorphine as well as administer long-acting injectable buprenorphine.
Since July 1st, 2023, ODT medicines have been listed on the PBS, becoming part of the Section 100 Highly Specialised Drugs (HSD) Program – (Community Access), with an accompanying funding programme to subsidise the daily dispensing fees associated with delivery of an ODT program in the community pharmacy setting. These changes will make ODT more affordable, lead to more people seeking treatment, normalise treatment as regular healthcare and increase locations for people seeking treatment.
As of July 1st 2024, community pharmacies can now dispense Section 100 HSD medicines, including ODT, under the Closing the Gap (CTG) PBS Co-payment Program. Alongside the PBS listing, this further supports access and reduces cost as a barrier for Aboriginal and Torres Strait Islander peoples accessing ODT.
Pharmacists must be aware of the changes and confident in providing the ODT Program.
- Factsheets and information on the PBS ODT Program are available here.
- More information on the Opioid Dependence Treatment (ODT) Community Pharmacy Program through the Pharmacy Programs Administrator (PPA) is available here.
State and territories run and operate their own ODT programs, which have individual policies, guidelines, and regulations that pharmacists must adhere to. Information for each state is available below.
References
1. Naren T et al 2022, Lifestyle interventions in the management of substance use disorder, Australian Journal of General Practice (AJGP), Volume 51, Issue 8, August 2022.
2. AIHW 2023, National Opioid Pharmacotherapy Statistics Annual Data collection, available from: https://www.aihw.gov.au/reports/alcohol-other-drug-treatment-services/national-opioid-pharmacotherapy-statistics/contents
Please refer to PSA’s NSW Opioid Treatment Program (OTP) – Foundation Training and Support website for more information.
1. Obtain an Opioid Dependency Treatment Centre Licence
To supply methadone or buprenorphine (including buprenorphine-naloxone), or administer long-acting injectable buprenorphine, pharmacists must apply to the Health Protection Service (HPS) to obtain an Opioid Dependency Treatment Centre Licence.
2. Familiarise yourself with the ACT protocols and guidelines
The Opioid Maintenance Treatment in the ACT: Local Policies and Procedures can be found in the pharmacist section on the ACT Health website, Opioid Maintenance Treatment.
All pharmacists dispensing treatment must successfully complete training for the safe administration and dispensing of opioid maintenance treatment. For information on course availability, please contact Canberra Health Services Alcohol and Drug Services.
Pharmacists are required to undertake refresher training delivered by ACT Health every 5 years.
3. Long-acting injectable buprenorphine
Pharmacists in the ACT may administer long-acting injectable buprenorphine (LAIB) as long as it is within their scope of practice and professional competency to administer, and in accordance with the prescription, as well as completing appropriate training. More information is available at: Pharmacist Vaccinations and Injectables, ACT Health.
Mandatory training requirements:
- If you are not a pharmacist immuniser, you must complete an accredited immunisation training course before administering medicines by injection.
- Complete the Opioid Maintenance Treatment in the ACT – Pharmacist Training Program provided by Canberra Health Services. For information on course availability, please contact Canberra Health Services Alcohol and Drug Services.
- Complete accredited clinical training on LAIB, which includes the PSA course: Long-acting injectable buprenorphine administration by pharmacists.
- This training is designed for appropriately trained pharmacist immunisers only.
- Undergo supervised practical injection training for administration of LAIB (this can be coordinated by Canberra Health Services or through a private prescriber/nurse).
Mandatory additional training:
- It is also mandatory that you complete the Administering medicines by injection course before administering any medicine by injection. Undergo supervised practical injection training for administration of LAIB. This may be facilitated using a blended model including – attend and observe a public clinic (Canberra Health Service, Alcohol and Drug Service at Building 7 at The Canberra Hospital can facilitate this via appointment only) or observe a private prescriber/nurse currently providing this service.
Other requirements:
- Be familiar, and practice in accordance with the PSA Guidelines for pharmacists administering medicines by injection
- Injectable services provided by pharmacists should only be provided in a safe, clean environment for the benefit of both the pharmacist and patient. These services should be provided in a closed consultation room.
- Pharmacists administering LAIB must electronically document the administration of the medicine and provide documentation to the patients LAIB prescriber.
4. Use language that reduces stigma
The language pharmacists use when providing Opioid Dependency Treatment is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
5. Provide relevant Self Care Cards to people seeking treatment for opioid dependence
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
6. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required.
Register for the Take Home Naloxone Program through the Pharmacy Programs Administrator (PPA) here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
7. Register for the Needle & Syringe Program
The Needle and Syringe program aims to minimise the transmission of blood borne viruses amongst people who inject drugs.
More information on the Needle & Syringe Program is available here, and locations/information on current providers is available here.
8. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
For specific advice on Opioid Maintenance Treatment, pharmacists can contact the Canberra Health Services Alcohol and Drug Services, Alcohol & Drug Intake & Helpline on (02) 5124 9977.
Keep up to date on the latest information on OTP programs in the ACT as well as many other important practice specific issues – renew your PSA membership!
1. Register your pharmacy details with the Queensland Opioid Treatment Program (QOTP)
If your pharmacy wishes to become involved in delivering this important public health program, email Queensland Health at QOTP@health.qld.gov.au with the following information:
- Pharmacy name
- Pharmacy business address
- Pharmacy phone number
2. Familiarise yourself with the QLD protocols and guidelines
Extensive information and resources are available on the QOTP website. Some key resources are outlined below:
- Queensland Opioid Dependence Treatment Guidelines 2023
- Fact sheet – Pharmacist Administration of Long-Acting Injectable Buprenorphine
- Queensland Health Departmental Standard – Monitored medicines
- Queensland Opioid Treatment Program
3. Long-acting injectable buprenorphine
Pharmacists in QLD may administer long-acting injectable buprenorphine as long as it is within their scope of practice and professional competency to administer. Pharmacists offering this service must be satisfied that the medicine will be administered safely to the patient.
Recommended training requirements:
-
- This training is designed for appropriately trained pharmacist immunisers only.
- If you are not a pharmacist immuniser, you must complete an accredited immunisation training course before administering medicines by injection and before completing the injection course.
- It is also recommended that you complete the Administering medicines by injection course before administering any medicine by injection.
Other requirements:
- Be familiar, and practice in accordance with the PSA Guidelines for pharmacists administering medicines by injection
- Pharmacies must have a consultation room that complies with the QLD Extended Practice Authority requirements.
4. Use language that reduces stigma
The language pharmacists use when providing Opioid Dependence Treatment is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
5. Provide relevant Self Care Cards to people seeking treatment for opioid dependence
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
6. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required. Register for the Take Home Naloxone Program here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
7. Register for the Needle & Syringe Program
The Needle and Syringe program aims to minimise the transmission of blood borne viruses amongst people who inject drugs.
Register for the Needle & Syringe Program here.
8. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
For specific advice on QOTP, pharmacists can contact the Queensland Health via email at QOTP@health.qld.gov.au .
The Alcohol and Drug Clinical Advisory Service (ADCAS) is a specialist telephone support service for health professionals in Queensland, providing clinical advice regarding the management of patients with alcohol and other drug concerns. This free service is available from 8.00am-11.00pm, 7 days a week. Contact at 1800 290 928.
Keep up to date on the latest information on OTP programs in QLD as well as many other important practice specific issues – renew your PSA membership!
1. Apply to become a Pharmacotherapy (opioid replacement therapy) Pharmacy
To make an application for permission to be a pharmacotherapy supplier, complete the application form available on the Victorian Department of Health website.
2. Complete the Victorian Opioid Pharmacotherapy Program (VOPP)
The aim of these training programs is to provide pharmacists and pharmacy support staff with the relevant knowledge, skills and tools required to deliver a safe and patient-centred Opioid Replacement Therapy (ORT) service.
- are fully funded by the Victorian Department of Health for all pharmacists and pharmacy staff in Victoria
- have all you need to know about delivering an ORT service
- help you establish your pharmacy to support patients with an opioid dependence
- enable you to play a key role in reducing the health, social and economic harms to individuals and the community
The VOPP will help pharmacists and pharmacy staff identify those who would benefit from pharmacotherapy, engage in a discussion of the benefits of the program in a non-stigmatising manner, and ensure the consistency and quality of services offered.
The LAIB training will enable pharmacist acquire relevant knowledge and skills to administer long-acting injectable buprenorphine in a safe and patient-focused environment.
The table below illustrates the training available to pharmacists to:
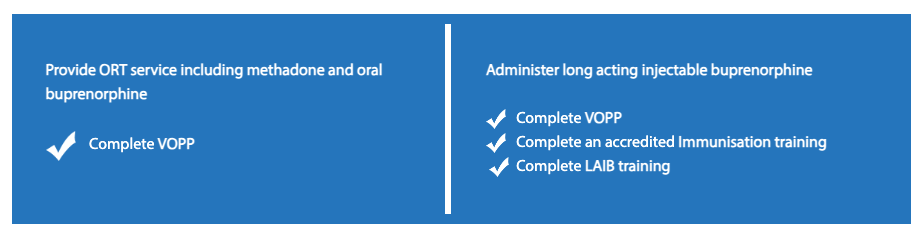
NB: VOPP is not a requirement to provide an ORT service, but highly recommended by the Victorian Department of Health.
NB: VOPP is not a requirement to complete the LAIB training but is highly recommended.
NB: An accredited injection administration training (i.e. the immunisation training) is a requirement to administer LAIB. The LAIB training is highly recommended, but not a requirement to provide LAIB in Victoria.
It is also recommended that you complete the Administering medicines by injection course before administering any medicine by injection, as well as, be familiar, and practice in accordance with the PSA Guidelines for pharmacists administering medicines by injection.
3. Familiarise yourself with the Victorian protocols and guidelines
Extensive information and resources are available on the Victorian Department of Health website. Some key resources are outlined below:
- Policy for maintenance pharmacotherapy for opioid dependence
- Pharmacotherapy policy addendum – Long-acting injectable buprenorphine
- Long-acting injectable buprenorphine – brief clinical guidelines
- Features of a Victorian pharmacotherapy prescription
4. Use language that reduces stigma
The language pharmacists use when providing opioid replacement therapy is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
5. Provide relevant Self Care Cards to people seeking opioid replacement therapy
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
6. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required. Register for the Take Home Naloxone Program here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
7. Register for the Victorian Needle & Syringe Program
The Victorian Needle and Syringe program aims to minimise the transmission of blood borne viruses amongst people who inject drugs.
Information on the Victorian Needle & Syringe Program is available here.
8. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
For specific advice on pharmacotherapy, pharmacists can contact the Victorian Department of Health at pharmacotherapy@health.vic.gov.au.
For clinical advice – the Victorian Drug and Alcohol Clinical Advisory Service (DACAS) is a 24/7 specialist telephone consultancy service that is free of charge for health and welfare professionals. Contact at 1800 812 804.
Keep up to date on the latest information on OTP programs in Victoria as well as many other important practice specific issues – renew your PSA membership!
If you would like to become involved in delivering Medication Assisted Treatment for Opioid Dependence (MATOD) services, contact the Drug and Alcohol Services Australia (DASSA) Community Pharmacy MATOD Program Manager (ph. 7425 5000 or email: HealthDASSAPharmacyEnquiries@sa.gov.au) for support, training and education.
1. Familiarise yourself with the SA protocols and guidelines
Extensive information and resources are available on the SA Health website. Some key resources are outlined below:
- Practice Standards for the Administration of Long-Acting Injectable Buprenorphine (LAIB) for South Australian Pharmacists are available here from 9 June 2025
- Community Pharmacy MATOD Program | SA Health
2. Long-acting injectable buprenorphine
From 9 June 2025, South Australian pharmacists can administer Long-Acting Injectable Buprenorphine (LAIB).
Adherence to the Practice Standards for the Administration of Long-Acting Injectable Buprenorphine (LAIB) for South Australian Pharmacists will ensure that individual pharmacists are working within their scope of practice and have all the requisite professional skills, relevant training, competencies and knowledge to administer LAIB.
3. Use language that reduces stigma
The language pharmacists use when providing Opioid Dependence Treatment is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
4. Provide relevant Self Care Cards to people seeking treatment for opioid dependence
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
5. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required. Register for the Take Home Naloxone Program here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
6. Clean Needle Program (CNP) Pharmacy Scheme
The Clean Needle Program (CNP) Pharmacy scheme aims to minimise the transmission of blood borne viruses amongst people who inject drugs.
Register for the CNP here.
7. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
For specific advice on MATOD from a regulatory perspective, contact the Drugs of Dependence Unit (DDU) on 1300 652 584 or at HealthDrugsofDependenceUnit@sa.gov.au.
For 24-hour clinical advice from senior medical staff, regarding opioid dependent patients and patients with other drug and alcohol related issues, contact the Drug and Alcohol Clinical Advisory Service (DACAS) on (08) 7087 1742.
Keep up to date on the latest information on OTP programs in SA as well as many other important practice specific issues – renew your PSA membership!
1. Apply to participate in the WA Community Program for Opioid Pharmacotherapy (CPOP)
If your pharmacy would like to become involved in delivering CPOP, complete the application form to start the process.
2. Familiarise yourself with the WA protocols and guidelines
Extensive information and resources are available on the WA Mental Health Commission website. Some key resources are outlined below:
3. Complete training provided by the Government of WA
All pharmacists working in CPOP pharmacies (including locums) are required to complete the CPOP Pharmacist Training provided by the Government of Western Australia Mental Health Commission. The training is available here.
4. Long-acting injectable buprenorphine (LAIB)
In Western Australia, this Structured Administration and Supply Arrangement (SASA) authorises a registered pharmacist trained in the CPOP to administer LAIB, when requested by the patient and prescriber. The conditions and criteria in the SASA must be met by the administering pharmacist.
It is expected that pharmacists are:
- familiar with and understand the requirements of the WA CPOP and the relevant SASA,
- understand requirements for injection administration by completing an injection/immunisation course approved by the Department of Health. If you are not a pharmacist immuniser, the PSA offers an approved accredited immunisation training course .
- understand the requirements specific to depot buprenorphine treatment and administration by completing the required training provided by CPOP.
It is the responsibility of the pharmacist to complete the expected training and product familiarisation to ensure that they are practising within their field of competency. It is also recommended that pharmacists:
- Complete the Administering medicines by injection course before administering any medicine by injection.
- Be familiar, and practice in accordance with the PSA Guidelines for pharmacists administering medicines by injection
5. Use language that reduces stigma
The language pharmacists use when providing pharmacotherapy is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
6. Provide relevant Self Care Cards to people seeking treatment for opioid dependence
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
7. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required. Register for the Take Home Naloxone Program here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
8. Needle & Syringe Program (NSP)
All Western Australian pharmacies are approved to retail packaged needles and syringes (Fitpack ® and Fitstick ®) under the Pharmacy Registration Board of WA’s approval.
Should a pharmacy want to retail single needles and syringes accompanied by a disposal container, the pharmacy is required to apply for an NSP approval to do so.
Apply for a NSP approval here.
9. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
The Community Pharmacotherapy Program (CPP) provides support, information, advice, training and resources for clients, pharmacists and medical practitioners involved in methadone and buprenorphine treatment for opioid dependence throughout WA. Contact via phone on (08) 9273 1907.
The Drug and Alcohol Clinical Advisory Service (DACAS), operating from 8am-8pm Mon-Fri, is a specialist telephone consultancy service that provides clinical advice to health professionals on all issues relating to patient management of alcohol and other drug (AOD) use. Contact on (08) 6553 0520.
Keep up to date on the latest information on OTP programs in WA as well as many other important practice specific issues – renew your PSA membership!
1. Dispensing Opioid Substitution Treatment
There are no specific requirements or authorisations for pharmacies/pharmacists to dispense Opioid Substitution Treatment in the NT.
It is recommended that pharmacists are familiar with the National guidelines for medication-assisted treatment of opioid dependence prior to providing this service.
2. Familiarise yourself with the NT protocols and guidelines
All information relevant to Opioid Substitution Treatment is available in the Schedule 8 Code of Practice. More guidance for pharmacists on restricted S8 substances is available here.
Some other useful resources are below:
- Summary of requirements for prescriptions for Schedule 8 Substances (S8s)
- Information for patients on S8 medications
3. Long-acting injectable buprenorphine
Pharmacists in the NT may administer long-acting injectable buprenorphine where instructed to by the prescriber. Pharmacists offering this service must be satisfied that the medicine will be administered safely to the patient.
- Recommended training requirements:
-
- Long-acting injectable buprenorphine (LAIB) administration by pharmacists
- This training is designed for appropriately trained pharmacist immunisers only.
- If you are not a pharmacist immuniser, you must complete an accredited immunisation training course before administering medicines by injection and before completing the LAIB course.
- It is also recommended that you complete the Administering medicines by injection course before administering any medicine by injection.
- Other requirements:
-
- Be familiar, and practice in accordance with the PSA Guidelines for pharmacists administering medicines by injection
4. Use language that reduces stigma
The language pharmacists use when providing Opioid Substitution Treatment is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
5. Provide relevant Self Care Cards to people seeking treatment for opioid dependence
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
6. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required. Register for the Take Home Naloxone Program here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
7. Register for the Needle & Syringe Program
The Needle & Syringe Program (NSP) aims to minimise the transmission of blood borne viruses amongst people who inject drugs.
Register for the NSP here.
8. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
For clinical advice – the Drug and Alcohol Clinical Advisory Service (DACAS) is a 24/7 specialist telephone consultancy service that is free of charge for health and welfare professionals. Contact at 1800 111 092.
The NT Department of Health Alcohol and Other Drugs Service can provide advice to pharmacists currently providing an ODT service or looking to implement this service. Contact at:
- AODTEHS.DoH@nt.gov.au, or
- 02 8922 8399
Keep up to date on the latest information on OTP programs in the NT as well as many other important practice specific issues – renew your PSA membership!
1. Obtain pharmacy approval and pharmacist accreditation to become a dosing site for opioid pharmacotherapy
Pharmacy Approval:
- To become a dosing site for opioid pharmacotherapy, a pharmacy requires approval from the Tasmania Alcohol and Drug Services (ADS). In addition, each pharmacist involved in the provision of dosing is required to obtain accreditation.
- To coordinate approval, contact the ADS on (03) 6230 7983.
Pharmacist accreditation:
- To dose pharmacotherapy, pharmacists require to undertake a short professional development program and exam.
- The ADS recommends this is completed in the intern year.
- If accreditation has not already been obtained, this will be coordinated by the ADS pharmacist.
2. Familiarise yourself with Tasmanian protocols and guidelines
Extensive information and resources are available on the Tasmanian Government Department of Health website. This includes:
- Tasmanian Opioid Pharmacotherapy Program Policy and Clinical Practice Standards
- Dosing sheets for community pharmacies
- Depot buprenorphine guidelines for pharmacists
- Medication administration charts
3. Long-acting injectable buprenorphine
Pharmacists in Tasmania may administer long-acting injectable buprenorphine after meeting mandatory requirements set out by the Department of Health. Detailed information on the requirements are available in the Pharmacist Administration of Depot Buprenorphine in the Treatment of Opioid Dependence Policy.
4. Use language that reduces stigma
The language pharmacists use when providing Opioid Substitution Treatment is critical to reduce stigma.
“The Power of Words practical guide and desktop flip book are designed to support healthcare and other professionals working with people who use alcohol and other drugs to reduce stigma and improve health outcomes.
Stigma is a common and complex problem for people who use alcohol and other drugs. The World Health Organization has ranked illegal drug dependence as the most stigmatised health condition globally, with alcohol dependence listed at number four.”
Download the Power of Words resource here.
5. Provide relevant Self Care Cards to people seeking treatment for opioid dependence
PSA self-care fact cards provide information for individuals about self-care and preventative health. The below fact cards provide information for individuals on drug overdose, methadone & buprenorphine, and safer injecting practices, as well as links to further resources and when individuals should seek medical attention.
- Drug Overdose
- Methadone and buprenorphine
- Safer injecting practices
The Self Care program is designed for pharmacies to deliver improved health care to consumers. It provides resources and training to educate pharmacy staff, add value to the consumer’s experience, and aims to increase business growth with tailored health promotions and resources. To learn more click the button below.
6. Register for the Take Home Naloxone Program
Opioid overdose is a major cause of harm and death in Australia. Naloxone is a short-acting opioid antagonist, registered by the TGA for the reversal of opioid overdose. Increasing access to naloxone for people who are at risk of experiencing or witnessing an overdose is an important strategy to prevent and respond to opioid harm and death.
The Take Home Naloxone Program fully subsidises the cost of naloxone, including dispensing fee, to participating community pharmacies. A PBS prescription is not required. Register for the Take Home Naloxone Program here.
Learn more about the naloxone and why you should talk to your patients about naloxone from Turning Point, Australia’s leading national addiction treatment, education and research centre.
7. Register for the Needle & Syringe Program
The Needle & Syringe Program (NSP) aims to minimise the transmission of blood borne viruses amongst people who inject drugs.
Register for the NSP here.
8. Pharmacy Incentive Program
To support community pharmacies to provide OTP services, the Tasmanian Department of Health has an incentive scheme for community pharmacies that provides additional funding. For further information, contact adstopp@dhhs.tas.gov.au.
9. Do you have more questions?
PSA Members can call the Pharmacist to Pharmacist Advice Line on 1300 369 772 for professional advice and support.
For clinical advice – the Drug and Alcohol Clinical Advisory Service (DACAS) is a 24/7 specialist telephone consultancy service that is free of charge for health and welfare professionals. Contact at 1800 111 092.
Keep up to date on the latest information on OTP programs in Tasmania, as well as many other important practice specific issues – renew your PSA membership!
